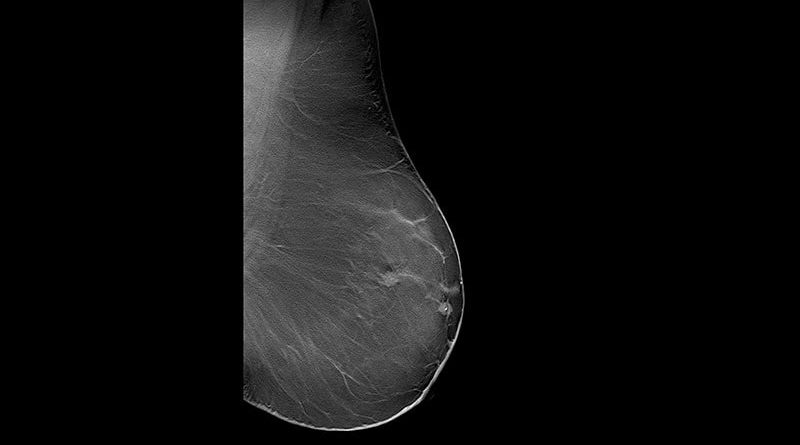
For Breast Cancer Screening, Tomosynthesis (3D) Beats Digital (2D)
Digital breast tomosynthesis (DBT), also known as 3D mammography, yields better breast cancer screening outcomes compared to standard digital (2D) mammography alone, concludes a huge retrospective study of more than a million women in the United States.
The cancer detection rate for DBT screening was 5.3 per 1000 patients screened, vs 4.5 per 1000 screened with 2D digital mammography only.
DBT screening was also associated with a lower rate of false positives and recalls.
“Our large, retrospective study further supports that digital breast tomosynthesis is the better screening mammogram,” said study co-author Emily F. Conant, MD, professor of radiology and chief of the Division of Breast Imaging at the Hospital at the University of Pennsylvania in Philadelphia.
“We showed that the major screening outcomes ― cancer detection rate, recall from screening, and cancers/biopsies recommended after recall ― were overall improved with digital breast tomosynthesis compared to screening with 2D mammography alone,” she added
Conant told Medscape Medical News that for mammographic screening for breast cancer, DBT should be the standard of care.
“But 2D mammography is, of course, still extremely important for diagnostic imaging, such as magnification views of concerning calcifications, etc,” she added. “So, we definitely don’t want to lose 2D digital mammography.”
The study was published March 14 in Radiology.
The first DBT system was approved in the US in 2012. Since then, this 3D technology has been replacing digital mammography as the preferred imaging modality for routine breast cancer screening, as previously reported in some detail by Medscape Medical News. The two technologies are being compared head-to-head in the randomized, federally funded Tomosynthesis Mammography Imaging Screening Trial (TMIST), but this study has enrollment problems in light of accumulating data showing the superiority of DBT.
This latest study shows that DBT is superior for all endpoints ― recall rates, cancer detection rates, positive predictive value of recall, biopsy rate, and positive predictive value of biopsy.
Conant and colleagues conducted a retrospective cohort study using data from five large healthcare systems across the United States. A total of 2,528,063 screening mammograms from 1,100,447 women (mean age, 57 years) were included in their analysis.
Most of the women included in the study had undergone at least two screening mammograms (digital, 82.4%; DBT, 81.7%), and roughly a quarter (23.6%) of mammograms were obtained for women who had been determined to be at elevated risk (digital, 23.6%; DBT, 23.5%).
Their results showed that compared with digital mammography, DBT had a significantly lower recall rate (10.3% vs 8.9%; P < .001), and this remained significant after adjustment for potential confounders (OR, 0.92; P < .001).
A total of 9714 cancers were detected during the study period (digital, 3421; DBT, 6293) from 1,948,098 screening mammograms. The postindex follow-up period was at least 6 months.
The overall crude cancer detection rate was better for DBT compared to digital mammography (4.5 of 1000 screening mammograms vs 5.3 of 1000; P < .001) and remained significant after adjustment for potential confounders (OR, 1.24; P < .001).
There was a higher positive predictive value of recall (4.3% vs 5.9%; P < .001) for DBT, and women who were screened with DBT had a higher rate of biopsy than women who were screened with digital mammography (17.6 of 1000 screening mammograms vs 14.5 of 1000; P < .001). However, the positive predictive value of biopsy was similar in both arms (29.3% vs 30.0%; P = .16).
Conant noted that the study has limitations, such as the “missingness” of some data and longer-term follow-up. “Prospective trials such as TMIST frequently have greater depth of patient-level data, such as longer follow-up, patient-specific morbidity and mortality, and often, more complete and detailed data on cancer biology and stage,” she said. “So, TMIST is also very important to drill down and answer some of these additional questions,” she added.
That DBT Is Superior Is “Not Surprising”
Approached by Medscape Medical News for comment, Daniel B. Kopans, MD, professor of radiology at Harvard Medical School, Boston, Massachusetts, noted that these results are not surprising. “The authors don’t state it, but a complete DBT screening study includes either full-field digital mammography [FFDM] 2D screening views or at least synthetic 2D screening views in both projections in addition to the planar information,” he said.
“Since every DBT screening study includes 2D images, there is no way that it can be worse than FFDM unless the planar information results in allowing a cancer visible on the 2D images to be ignored. Consequently, DBT can only be equal to or better than FFDM performed alone.”
Kopans pointed out that the major problem with this and all the other studies that compare FFDM to DBT. “The investigators and those reading the mammograms have no way of knowing why some women had FFDM and why others were chosen to have DBT,” he said. “It was likely not a random assignment, and there could be unknown selection biases.”
He surmised that the ideal study would be prospective, and it would be one in which the technologists obtained FFDM images and the DBT planes, but the radiologists first read the 2D images without the planar images and then locked the report into the computer. “Then the reader would go back and add in the planar images and issue a second report,” Kopans said. “At this point, such a study is not necessary since everyone who has used DBT routinely for screening knows that it finds cancers that are not visible on the 2D images, even in retrospect.”
Adds to Literature, With Limitations
Two other experts also note limitations of this study in an accompanying editorial. Min Sun Bae, MD, from the Department of Radiology at Inha University Hospital, Incheon, Republic of Korea, and Bo Kyoung Seo, MD, from the Department of Radiology, Korea University Ansan Hospital, Ansan, Republic of Korea, note that this “large population-based study adds to the existing literature on improved performance of DBT screening.”
But there are limitations, as it is a retrospective observational study with data from the transition from digital mammography to DBT. They point out that the investigators used data from women who had undergone screening with digital mammography in an earlier period and those screened with DBT in a more recent time. “This is not an absolute comparison between digital mammography and DBT in the same cohort,” they write. “Additionally, as the authors pointed out, data on some baseline characteristics (eg, breast density, race, menopausal status, and screening interval) were unavailable for substantial proportions of screening mammograms.
“The analysis of additional measures, such as the advanced cancer detection rate and the interval cancer rate, will help clarify the impact of DBT screening on clinical outcomes,” they conclude.
Conant has received institutional grants from iCAD, consulting fees from iCAD and Hologic, payment for lectures from Hologic, Medscape, and Aunt Minnie, and support for travel to meetings from the RSNA. He has an unpaid leadership role with the Society of Breast Imaging. Kopans is a consultant for DART Imaging; he was the inventor of digital breast tomosynthesis but no longer holds patents on the technology. The editorialists have disclosed no relevant financial relationships.
Radiology. Published online March 14, 2023. Full text, Editorial
Roxanne Nelson is a registered nurse and an award-winning medical writer who has written for many major news outlets and is a regular contributor to Medscape.
For more news, follow Medscape on Facebook, Twitter, Instagram, and YouTube.
Source: Read Full Article