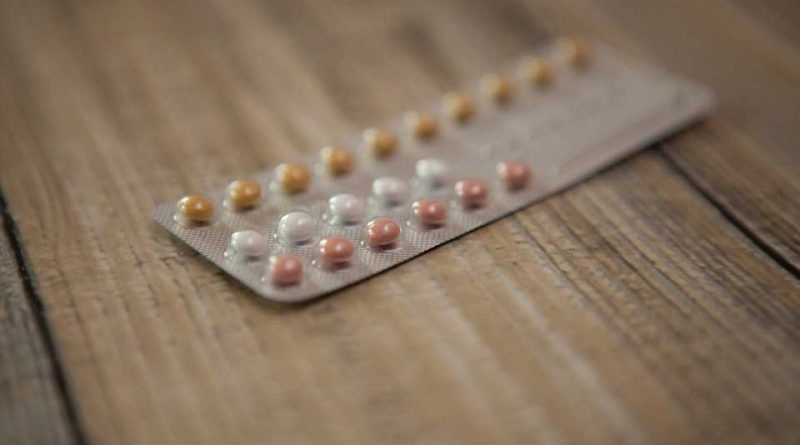
How does the new OTC birth control pill, Opill, work to prevent pregnancy? 5 questions answered
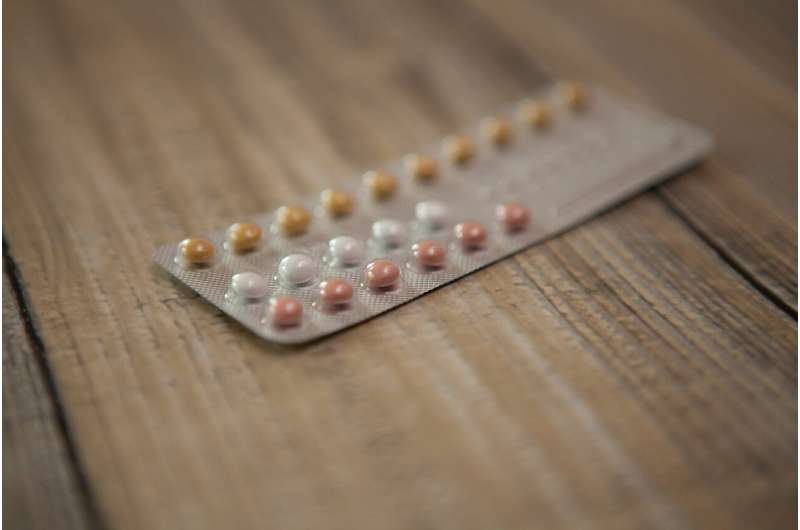
The Food and Drug Administration’s July 13, 2023, approval of the first over-the-counter birth control pill, called Opill, broadens the options for people seeking to prevent pregnancy. When Opill becomes available, presumably in the first quarter of 2024, it will be sold in grocery and convenience stores, in pharmacies and through online retailers.
The Conversation asked Sarah Lynch, a pharmaceutical expert from Binghamton University, State University of New York, to answer some of the key questions people have about the new over-the-counter contraceptive.
1. How does Opill work to prevent pregnancy?
Opill contains norgestrel, which is a synthetic form of the hormone progesterone. Progesterone works in several ways to prevent pregnancy. First, it thickens the mucus in the cervix, which makes it challenging for sperm to enter the uterus and fertilize an egg. Second, it thins the lining of the uterus, making it less hospitable for a fertilized egg to implant. And third, it can prevent ovulation, or release of the egg, in most people.
Opill, like many other progestin-only birth control pills, must be taken at the same time each day to prevent pregnancy. This is because progestin has to stay at a certain level in the body in order to effectively prevent pregnancy.
If an Opill dose is taken even three hours late, or if vomiting or diarrhea occurs within four hours of taking the dose, a person should avoid intercourse or use some form of nonhormonal contraceptive method for two days. Even though it only takes about two days for the drug to build up to an effective level, sperm can remain fertile in the female reproductive tract for up to five days after intercourse, meaning that it is important to take this medication regularly both before and after unprotected intercourse.
When used exactly as instructed, Opill is 98% effective. This makes it the most effective contraceptive option available for use without a prescription. Opill does not prevent sexually transmitted infections, so people looking to further protect themselves should still use some sort of barrier method during intercourse.
2. Is Opill safe to be sold over the counter?
Prior to Opill’s approval in the United States, birth control pills were already available without a prescription in more than 100 countries around the world. The same drug in Opill, norgestrel, has been used safely and effectively for birth control since 1973. It has been available by prescription under the brand name Ovrette.
In order for a drug to be sold without a prescription in the U.S., it must first be reviewed and approved by the Food and Drug Administration. The FDA ensures that the product can meet several conditions for safe use: It must be able to be used appropriately by consumers for self-diagnosed conditions, it should not need a health practitioner for safe and effective use, and it must have a low potential for misuse and abuse. The FDA also requires that over-the-counter drug manufacturers follow specific labeling requirements and include information about the drug’s use, warnings, purpose and directions.
Norgestrel has been shown to be safe for most women. However, it should not be used by those who currently have or have ever had breast cancer, because some breast cancers are hormone-sensitive and in some cases, hormones lead to increased growth of tumors. People should also not use Opill if they are pregnant or are taking certain medications used for seizures, tuberculosis, HIV/AIDs or pulmonary hypertension because norgestrel may not work as effectively when taken with these medications.
Several studies have looked at whether women can accurately evaluate their own ability to safely use birth control. The studies show that women are accurate in their evaluations and may take birth control pills for a longer period of time when compared to having a doctor evaluate and prescribe for them.
3. Shouldn’t a doctor be involved in choosing birth control?
Getting a prescription for any type of hormonal contraceptive product has traditionally required a medical appointment and a screening examination with a health care provider. Screenings may include pap test, pelvic examination, clinical breast examination and testing for sexually transmitted diseases. Although important, leading medical organizations such as the American College of Obstetricians and Gynecologists state that these screenings are not required before safely using hormonal contraception.
Even before the approval of Opill, people had the option to uncouple their screening examinations from prescription access. One way has been through telehealth. A 2018 review of several online telehealth platforms found that these companies are still able to screen for safe use and provide safe birth control recommendations without any type of in-person examination. In addition, more than 20 states currently allow pharmacists to provide prescription contraceptive based on a self-assessment questionnaire and blood pressure screening.
People who want to use any type of nonprescription medication should ensure that they know their medical history and what medications they take. They should carefully review the labeling information and, if they have questions, ask their pharmacist or reach out to their primary care provider.
4. Does Opill have any side effects?
Some of the most common side effects of Opill include nausea, breast tenderness, increased appetite, acne, fatigue and headaches, which are similar to the side effects of other hormonal birth control products. With most hormonal contraceptive products, these side effects diminish over time.
Opill does not contain estrogen, as some other hormonal birth control pills do. Estrogen plays a role in menstrual regularity, so people who use Opill may experience more irregular vaginal bleeding. But some individuals who use Opill may have less bleeding or stop bleeding altogether while taking the pills.
A commonly raised concern regarding safety of hormonal birth control is the risk of blood clots, such as deep vein thrombosis or pulmonary embolism. This risk is mainly associated with products that contain estrogen in addition to progestin.
Progestin-only pills such as Opill carry no or minimal risk of blood clots. However, even products that contain estrogen still have a lower risk of blood clot than the risk during pregnancy or the postpartum period.
5. Will OTC status truly increase accessibility to birth control?
Over-the-counter availability of Opill will undoubtedly increase access to those who are looking to prevent pregnancy without access to, interest in or time to see a health care provider.
However, cost constraints may still be an issue with Opill. The cost is unknown at this time. The Affordable Care Act currently mandates insurance coverage of certain FDA-approved prescription birth control products, but it does not require coverage of nonprescription options. In May 2023, lawmakers reintroduced legislation requiring coverage of over-the-counter options, which would require that private health insurance plans cover FDA-approved over-the-counter contraceptives without a prescription.
Lastly, Opill represents only one type of birth control. While Opill was 98% effective under “perfect-use” conditions in the clinical trials of the drugs, birth control pills generally have an effectiveness of between 91% to 93% under “typical-use” conditions. “Perfect use” applies to using a method consistently and correctly, while “typical use” represents effectiveness among all people who use the method, including those who do not use it consistently or correctly. Effectiveness rates of contraceptives are measured in contraceptive failure. If 100 women use a birth control that is 91% effective over one year, it is estimated that nine women using that method will become pregnant over that year.
People looking for options that don’t need to be taken daily and as precisely, include different hormones or provide other noncontraceptive benefits will need to continue to rely on prescription products at this time.
Provided by
The Conversation
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Source: Read Full Article